- Mail us: support@drtimpearce.com
Does fear of managing tear trough complications keep you awake?
You may be interested
 Dr Tim Pearce
Dr Tim Pearce

Aesthetic practitioners can become quite anxious about performing certain medical aesthetic procedures, and none more so than treating the tear trough with soft tissue fillers.
Conquering those fears is something that we can help with as Dr Tim Pearce takes you on a journey of avoiding, managing, and treating complications and adverse effects from under-eye fillers, including the dreaded periorbital oedema.
Dr Tim regularly discusses medical aesthetic training tips in his weekly webinar, so if you’re looking to increase your CPD-certified learning and want reassurance about how you’re treating patients, then step one is to register for Wednesday’s free webinar by Dr Tim.
Is it normal to have swelling after tear trough filler treatments?
The simple answer is yes. It is completely normal for a patient to experience a post-procedural reaction to filler treatment under the eyes in the form of periorbital oedema or swelling. The skin in the tear trough is so thin that periorbital oedema, erythema (redness) and bruising will all likely occur. This must be explained clearly to patients to avoid anxiety post-treatment. Swelling will happen, but it only becomes a problem for you, and your patient, if it persists or suddenly appears after some delay.
Patients will often ask; how long does it take for tear trough filler treatment to settle? The thought of wandering around potentially looking like you’ve had too many late nights or been in a fight, especially if there’s bruising, does not generally appeal to patients, so your first job is to appease their concerns regarding this treatment.
Avoiding common complications with tear troughs
Preventing complications, such as periorbital oedema with tear trough filler treatments is the holy grail for all aesthetic practitioners, let’s face it, in an ideal world you would not need to manage any complications if you could avoid them completely. That’s why we developed our dermal filler complications mastery course.
There are some key considerations which will help you in your management and avoidance of complications from periocular fillers.
- Patient selection – If a patient reports waking up most days with puffy eyes and general swelling around the under-eyes first thing in the morning, then it is worth questioning whether you want to treat their tear trough. The area is already sensitive to fluid build-up so any additional fluid draw from the action of the filler will make the area look even more obvious.
- Production selection – Choose your product wisely, not all products are suitable for use in the periorbital area. If a soft tissue filler product – and we are referring to hyaluronic acid-based products only here – is designed to hold a lot of moisture and provide significant volume, it will be great for use in the cheeks but is not the right product for use in the tear troughs. Dr Tim recommends using Teosyal Redensity III which has a U.S. FDA approval for treatments in the under-eye area, or Juvéderm Volbella.
- Injection technique – As you learn and increase your skills with injecting dermal fillers you will start to recognise different patient types and be able to modify your injection technique accordingly to reduce any risks of both complications or undesirable results.
Will using a cannula or needle for tear trough treatment increase the risk of causing under-eye swelling?
There is much debate about whether to use a sharp needle or blunt cannula when performing soft tissue filler treatments in the tear trough.
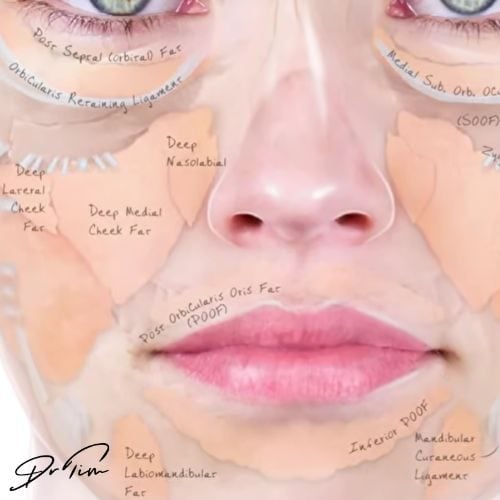
A cannula is used more superficially meaning that it is more likely that the filler product will be placed in the Sub-Orbicularis Oculi Fat pad or SOOF. This will mean that there is a mixture of filler and fat, making the filler more mobile as it attracts moisture, this increases the risk of periocular oedema.
By contrast, a needle can be used to place product more deeply, down on the periosteum or bone surface, meaning that the filler will be below the fat, pushing it up and propping up the tear trough area. Delivery of treatment by sharp needle will reduce the chances of causing bruising and oedema, or that “I’ve-been-in-a-fight-look”, as the filler is placed much deeper.
What causes periorbital oedema?
The primary cause of swelling after dermal filler treatment in the tear troughs is simply post-procedural. Nine times out of ten, if the swelling happens quickly, then this is caused by the natural body reaction to a needle or cannula entering the skin, in what is a sensitive area.
Similarly, bruising caused during treatment can also initiate swelling, both of which are normal inflammatory reactions, rather than periorbital oedema per se. The best thing you can do is wait. Most cases will settle within a week. This can, of course, be unsettling for the patient and you will need to reassure them that you are allowing it to settle and their upset will be short-lived once the results reveal themselves.
It is also worth mentioning that the filler itself may be causing the swelling. Soft tissue filler products are designed to attract fluid, as is the nature of hyaluronic acid, but they can also impede the lymphatic drainage in the area, depending on product placement. Spotting this and massaging the area to move a bolus of filler, releasing fluid build-up, and aiding natural drainage can be a quick and simple solution. Why not watch this simple video which shows you the technique that Dr Tim uses to manage oedema after tear trough filler using massage. If there is no sign of inflammation or tenderness, then massage is also a good option to relieve swelling if it is still present 1-2 weeks after treatment; you can even show patients how to do this themselves at home to resolve the fluid retention.

Remember, oedema in this area is not always a reaction to the dermal filler product and you do not need to immediately reach for the hyaluronidase. Some patients do react to filler products and may need steroids and emergency hyaluronidase but avoid this being your first diagnosis. If you rush to use Hyalase™ in these situations you risk making things worse by creating more bruising delivering the hyaluronidase when all that was needed was time. The patient will not thank you if you make them look even worse out of a misguided need to solve the post-procedural swelling.
If the oedema is prolonged or delayed, plus erythematous and painful, then you also need to consider infection. This usually manifests on one side, making it easier to spot, although patients do sometimes just experience increased water retention on one side of their face. However, if you have unilateral redness and tenderness, the likely complication is an infection and not a reaction to the product.
If you have exhausted all options – leaving it and waiting for a week or so, massaging, checking for and treating infection – and periorbital oedema is still a daily presence, then you can consider hyaluronidase as your final course of action. You can then either try the treatment again with the patient’s consent or consider alternative strategies to address their under-eye concerns. If you need help with using Hyalase™, please download the guide to elective dermal fillers reversal protocol.
Are you still anxious about performing medical aesthetic treatments?
If you want to learn more about mastering medical aesthetic treatments or conquering the anxiety of preventing and treating complications, then register for Wednesday’s webinar on how to free yourself from complications anxiety.
Related Articles
 Bestseller
Bestseller
Why PRP Doesn’t Work The Same For Everyone
May 12, 2026











Comments (6)
Barbara
Oct 02, 2020Have you had any patients with severe reactions due EBV or mold toxicity.
Ashley Scott
Oct 06, 2020Hi Barbara, I’m afraid we haven’t.
Paronetto Anabella
Aug 14, 2020very good course!
Ashley Scott
Aug 18, 2020Hi Paronetto, thank you for the feedback, it’s always great to hear when people have found our content helpful.
June Dickson
Jul 26, 2020Fabulous course
Ashley Scott
Aug 18, 2020Hi Jackie, thank you so much for the kind feedback, I’m really pleased to hear you found it useful.
Comments are closed.