- Mail us: support@drtimpearce.com
5 early warning signs of a vascular occlusion when injecting fillers
You may be interested
 Dr Tim Pearce
Dr Tim Pearce

Early diagnosis of a vascular occlusion (VO) is crucial for ensuring the best outcome for your patients. Unfortunately, aesthetic clinicians often make some common mistakes that hinder early detection of VOs. These include, misdiagnosing it as herpes simplex, delaying seeing the patient for evaluation, and neglecting to educate patients about what is considered normal discomfort versus abnormal pain, leaving them unaware of potential warning signs and a reason to contact their practitioner.
In this blog, Dr Tim Pearce will explain some of the early warning signs, covering areas including pain during injection, pallor, livedo reticularis, post-procedural pain, and blistering on the skin. He also covers why capillary refill checks are vital and tips to help you to reduce your chance of experiencing a necrotic injury from vascular occlusion.
Do you feel anxious about causing complications? Many clinicians feel so overwhelmed with the thought of causing a vascular occlusion that it stops them growing their aesthetics business. Dr Tim is currently hosting a webinar series to help you overcome your fear of complications so that you can uplevel your knowledge, and increase your CPD-certified learning to build a successful aesthetics business. Sign up here >>
How can the delayed diagnosis of a vascular occlusion cause necrotic injury?
Dr Tim recalls that the worst necrotic injury he has ever seen was caused entirely by delayed diagnosis. The patient contacted the clinic within three hours of the procedure and explained that she thought there was something wrong. The clinic reassured her that it was normal to feel pain after a procedure. She telephoned them again, still concerned, and was given similar reassurance. When blisters started to appear on the skin, the same clinician diagnosed cold sores. Eventually, the patient was in so much pain that she went to an Accident & Emergency department for assistance. There, she was treated for a skin infection. Time continued to slip away whilst hyaluronidase was not administered to halt the impact and reduce the continued damage being caused by the filler that was blocking the blood supply. One small mistake at the start of this case led to a necrotic injury, aside from the procedure itself. This is so easily avoidable with systematic thinking that can reduce the time between the blockage of the vessel occurring and diagnosis of a vascular occlusion, leading to prompt action by dissolution before necrosis can happen.
Let’s look at the warning signs that can help you diagnose a vascular occlusion in your patients quickly.
Vascular occlusion warning signs (1): pain during injection
 The earliest possible warning sign that something is not right is pain when you inject, explains Dr Tim. In the many cases of vascular occlusion that he has reviewed as an aesthetic trainer, the first sign has been reported by the patient as a particularly painful injection. Of course, all injections hurt a little bit, but the key is to try to gauge with a particular patient whether one injection feels disproportionately more uncomfortable or painful for them. This is not the most sensitive test, but in retrospect, it often becomes obvious to both patient and practitioner that the causal injection was different.
The earliest possible warning sign that something is not right is pain when you inject, explains Dr Tim. In the many cases of vascular occlusion that he has reviewed as an aesthetic trainer, the first sign has been reported by the patient as a particularly painful injection. Of course, all injections hurt a little bit, but the key is to try to gauge with a particular patient whether one injection feels disproportionately more uncomfortable or painful for them. This is not the most sensitive test, but in retrospect, it often becomes obvious to both patient and practitioner that the causal injection was different.
Dr Tim’s advice would be to stop injecting if you feel that an injection is hurting differently to others you have administered on the same patient. Once the needle is removed, check capillary refill, ensure the patient is not haemorrhaging from the injection site – this is another sign that you have gone through a vessel – and consider choosing a slightly different position for subsequent injections in the same place.
Vascular occlusion warning signs (2): pallor
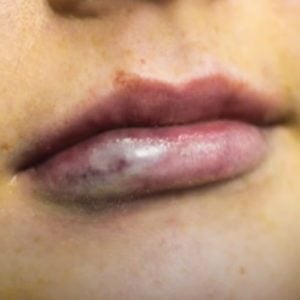
After the initial injection, the next sign of a problem with a VO is usually pallor. In the case of a true, complete vascular occlusion, pallor is very stark, particularly in lips. There will be a grey patch on the lip that sometimes has zero capillary refill. This is the most obvious type of VO and not easily missed in lips; however, they can be less obvious and more easily missed in other parts of the face, or in patients with darker skin types.
When it comes to diagnosing, Dr Tim notes quite a high degree of false positives with patients who get a degree of pallor but who do not have a VO. This occurs after lidocaine anaesthetic cream is used on the lips and they can become blotchy. Similarly, the procedure itself can cause blotchiness which often confuses both patients and clinicians into thinking that they have a vascular occlusion. If you look very closely with this type of pallor, the capillary refill is still present and within two seconds, the tissue is simply paler. You can compress the lip, recheck, and if you see within the heart of the pale area a little bit of capillary fill, it is probably just blotchiness from the anaesthetic. Another clear sign for differential diagnosing is that it does not fit the path of a blocked artery. If both the top and the bottom lips look blotchy, it is very unlikely that you have occluded both labial arteries, thus, you can readily suspect that the pallor is because of the lidocaine effect.
Pallor does not last for very long and is an early sign which normally gives way to the next warning sign, livedo reticularis.
Vascular occlusion warning signs (3): livedo reticularis
Livedo reticularis is a net-like pattern or a blotchy, purple rash that is associated with the disruption in the blood drainage of the skin. The venules might still be taking blood away from the skin, but the arteries are not replacing it. This creates pale patches next to darker patches leaving a blotchy appearance and is usually associated with larger vascular occlusions.
Livedo reticularis appears within minutes, rather than seconds, with blotchiness commencing perhaps 15 to 30 minutes after the procedure. It is very much an indication that the patient should be seen by the practitioner straight away.
Vascular occlusion warning signs (4): post-procedural pain
The next warning sign associated with a vascular occlusion is post-procedure pain. Post-procedural discomfort is quite normal, most patients will describe an ache or mild discomfort after a large procedure in most places where they were injected. However, if there is an area of localised pain that seems much worse than anywhere else and requires the patient to consider taking strong painkillers to cope with the pain, this would be a trigger that they need to be seen straight away by the clinician.
Dr Tim cautions that he has come across several cases where patients were not informed that significant post-procedural pain could be a sign of a VO. Thus, they thought it was normal, took painkillers, went to bed, and woke up nine hours later with a much-progressed vascular injury.
Ensure your patients understand the difference between discomfort and pain. Discomfort in the form of tenderness, particularly when an area is pressed is very normal after a procedure, but pain that is building and throbbing in one place is not normal and the patient should be seen.
Vascular occlusion warning signs (5): blistering skin
Blistering skin is the next warning sign of a vascular occlusion and is notorious for causing confusion amongst aesthetic practitioners.
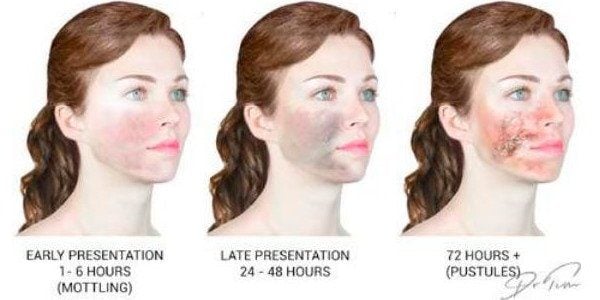
Commonly, the blisters are mistaken for herpes simplex or the cold sore virus. Herpes simplex blisters are usually a pale-coloured blister, whereas, when there is a necrotic wound, and the tissue is breaking down, there will be more pustules or yellowy blisters present. These blisters also tend to be in the path of the artery and far less likely to affect the white lip than the pink lip.
If a patient complains of the appearance of blisters post-procedure, you should check their location (ask for a photograph) and check the patient’s medical history in relation to past outbreaks of herpes simplex. This will allow you to diagnose consistency with a simple outbreak versus a completely new event presenting with different coloured blisters in line with the vasculature in the area treated that is an early stage of skin breakdown caused by VO.
Take home message
The single, most powerful way to quickly discover and diagnose a vascular occlusion is to check capillary refill on all patients, says Dr Tim. Do this during the procedure and not just at the end.
As well as understanding all the early warning signs yourself, as an aesthetic clinician, it is vital that you teach your patients what to look out for too. Do not be concerned that if you tell your patients about vascular occlusions that they will not have the procedure. This is about trust. If you convey confidence and certainty when describing a vascular occlusion, how you will avoid it, and what you will do if one happens, you will likely have more patients than the average aesthetic clinician because you know how to handle the risk and patients will believe in you.
Get more insight from Dr Tim by reading his blogs:
- Blogs on Dermal filler safety: vascular occlusion and necrosis prevention, and High risk areas, non-reversible fillers & vascular occlusion prevention.
- Reviewed of learning points from a very interesting case of earlobe vascular occlusion
- Managing a VO vascular occlusion: how much Hyalase (Hyaluronidase)?
You can find Dr Tim Pearce on Instagram if you have any questions or comments about avoiding or treating vascular occlusions..
Aesthetics Mastery Show
5 Early Warning Signs of a Vascular Occlusion
Dr Tim says:
“Diagnosing a vascular occlusion (VO) early is crucial for ensuring the best outcome for your patients. Unfortunately, I often witness clinicians making common mistakes that hinder early detection. These mistakes include misdiagnosing, delaying patient evaluations, and neglecting to educate patients about what is considered normal versus abnormal, leaving them unaware of potential warning signs. So, in this episode I discuss 5 early warning signs of a vascular occlusion so you can make informed decisions and act quickly if necessary. “
Watch the full Aesthetics Mastery Show here.
Is your worst nightmare causing a VO?
If you want to be a great injector then you need to get over your fear of complications. Register here for the next webinar to help you overcome your complications anxiety >>
Subscribe to our YouTube channel for really useful regular tips and advice. ![]()
Complications eLearning Course
Dermal Fillers
If you want to increase your confidence by learning how to handle complications, Dr Tim Pearce offers a comprehensive course Dermal Filler Complications Mastery. This includes CPD and certificates on completion.
In addition, browse our FREE downloadable resources on complications.
Dr Tim Pearce eLearning
Dr Tim Pearce MBChB BSc (Hons) MRCGP founded his eLearning concept in 2016 in order to provide readily accessible BOTOX® and dermal filler online courses for fellow Medical Aesthetics practitioners. His objective was to raise standards within the industry – a principle which remains just as relevant today.
Our exclusive video-led courses are designed to build confidence, knowledge and technique at every stage, working from foundation level to advanced treatments and management of complications.
Thousands of delegates have benefited from the courses and we’re highly rated on Trustpilot. For more information or to discuss which course is right for you, please get in touch with our friendly team.
Related Articles
 Bestseller
Bestseller
Deep Fat Pads: Understanding Facial Volume Architecture for Natural Dermal Filler Results
April 23, 2026
 Bestseller
Bestseller
Why Everything we’re Doing for Skin, Hair, and Weight May Not Translate Clinically
April 21, 2026













