- Mail us: support@drtimpearce.com
6 Lip Filler Safety Tips: How to Avoid Lip Filler Complications
You may be interested
 Dr Tim Pearce
Dr Tim Pearce

When clinicians first start injecting in medical aesthetics, they often get most excited about treating lips, but then as soon as they get going after completing a training course, they start to realise that the risks of treating lips are quite high. This is when the anxiety kicks in!
In this blog, Dr Tim Pearce will answer questions posed by practitioners and offer safety tips that will help you to achieve beautiful results when treating lips with dermal fillers, without causing subsequent problems including bruising, lumps, or vascular occlusion (VO).
Do you feel anxious about causing complications? Many clinicians feel so overwhelmed with the thought of causing a vascular occlusion that it stops them growing their aesthetics business. Dr Tim is currently hosting a webinar series to help you overcome your fear of complications so that you can uplevel your knowledge, and increase your CPD-certified learning to build a successful aesthetics business. Sign up here >>
1/ What is the maximum amount of dermal filler you can add in one treatment session while remaining safe when treating lips?
Dr Tim explains that he believes you should never use more than 1ml of dermal filler in the lips per treatment session, even though some practitioners do use more. His rationale is that there is a risk that adding too much at once may be a bit of a shock to a patient, you may get a bad aesthetic result, and it is better to do things gradually – take time to think and observe what you did using a follow-up appointment, reassess and then you can add more in a controlled way if required. But that is not all, if you add too much all at once, there is a chance that you can invert the wet-dry border, which results in the patient constantly licking their lips to keep them wet. Plus, there is a small risk of vascular compression or lumpiness from too much filler delivered in one injection.
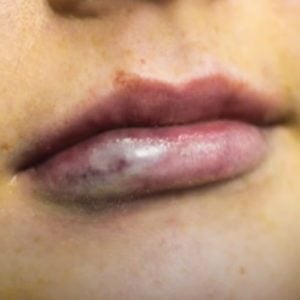 2/ What are the risks of vascular occlusion in the lips and how can we avoid causing a VO?
2/ What are the risks of vascular occlusion in the lips and how can we avoid causing a VO?
The risk of causing a vascular occlusion in the lips is rather high, but the severity of such VOs tends to be lower than in other areas of the face for two main reasons. Firstly, a vascular occlusion in the lips is usually diagnosed quickly because you can see when the lips have a compromised blood flow, therefore, treatment for a VO normally happens earlier and the rescue processes are usually more effective. Secondly, we do not tend to be using very large volumes of filler in the lips, thus any occlusions will be smaller – Dr Tim prefers to place approximately 0.05ml per injection point.
There are many things that you can do to reduce the risk of causing a vascular occlusion, but if he wanted to give you one top tip, Dr Tim would say,
“think about the anatomy in millimetre-by-millimetre detail”.
You need to have an awareness of the depth of your injection. If you are very deep, and particularly close to the vermilion border, that is where the superior labial artery lies, which tends to be the area that gets occluded the most often. If you are more superficial and you are doing little depth checks, you get the idea of where your needle is positioned much more clearly. The most important factor to be aware of is your depth relative to the superior labial artery.
3/ How deep can you inject the lips while staying safe?
The superior and inferior labial arteries tend to be approximately 3-5 millimetres underneath the vermilion border (from the surface of the skin), both on the top and the bottom lip, so this is the highest risk area. If your needle is not that deep (less than three millimetres), then you should be further away from the artery, but there are other things you can do before you inject to decrease your risk.
- Look for the artery before you start injecting – occasionally you can see it in the lip
- Feel for it
- Inject small amounts at a time
- Aspirate
If you are injecting the body of the lip, there is more room to be deeper than 3mm. However, you must still visualise where the superior labial artery lies – usually just underneath the orbicularis oris muscle and curving upwards. If you are injecting the lip body of a patient who is young with full lips, you will have more room than if you are injecting a patient who is older with thin lips, or someone who has small lips. In which case, you need to be particularly sensitive about the position of your needle tip as you are going down the anterior wall of the lip because you are getting closer to that area underneath the muscle which is where the labial artery lies 80% of the time.
 4/ Should you avoid treating the part of the vermilion border that is in between the Cupid’s Bow?
4/ Should you avoid treating the part of the vermilion border that is in between the Cupid’s Bow?
This area that is dead centre in the middle of the lip is sometimes called the middle cubicle, but not every patient will have one.
Anatomically speaking, the middle of the lip is riskier to treat because blood vessels come across the area laterally and become fractionally more inferior and closer into the lip body.
Aesthetically speaking, there is less reason to treat the middle of the lip and focus is better placed on treating the lips laterally. There will, however, be some patients with a middle cubicle that requires some augmentation after you have addressed the lateral points. Yet, Dr Tim believes that your average patient probably does not need injections in this area. He has seen some practitioners injecting right down to augment the cupids bow but believes that this sometimes has the opposite of the desired effect. If you are injecting along the vermilion border, medially between the Cupid’s Bow, instead of creating an arch where the Cupid’s Bow becomes more prominent, it will result in you filling the middle and losing some of that shape.
5/ I’m an experienced injector, but I still end up getting lumpy lips. How can this be?
Assuming that your patients are not suffering from an allergic reaction which would be out of your control, there are lots of factors that can contribute towards the occurrence of lumps when treating lips.
Firstly, we can consider how much filler product you are placing in each bolus – the more you put in with one injection, the more likely it is that your patient will see and feel the filler, as a lump.
Secondly, we must consider the product that you are using, is it one that is more likely to cause lumps? Contemplate trying different dermal filler products, particularly softer gels, and the lip results might improve.
Thirdly, are you massaging your patient’s lips after you have treated them? Dr Tim states that massage is about 50% of the work when you are injecting lips, and a simple massage in between your injections or at the end of every procedure should dramatically reduce your risk of lumpy lips. Feel, squeeze, massage and smooth along the lips gently as if you are sculpting with Plasticine to ensure they are the shape that you want. Caution: do not squeeze product into the white lip.
6/ How can you avoid bruising when injecting lips?
The simplest method for reducing bruising is to reduce the number of entry points for the needle. Every time you place the needle into the lips, you are going to penetrate tissue, and some will contain blood vessels that will bleed. The more often you go into lips with your needle, the more bruising you will cause. Review your technique and treatment plan to ensure you deliver the filler into the lips in the most efficient way, avoiding unnecessary injection points.
Another influence on bruising is being in control of your movements. More experienced injectors learn that it is very important that you become firm in your body before the needle enters the patient’s skin – ensuring that you are stable from your feet upwards.
Starting with your feet fixed and splayed apart, pelvis resting on the bed or couch, your forearm also resting on it, and your hand resting on the patient’s face, sometimes also with your finger stabilising so that the only muscles that you must control are in your fingertips. This gives you precision and an increased ability to control finer movements, meaning that you are not going to penetrate unnecessarily deeply or with a lack of control that could cause bruising.
Additionally, the temperature of your clinic room can impact on your patient’s chance of bruising, particularly on hot summer days. Heat and vasodilation employed by the body to keep cool can dramatically affect how much blood is in your patient’s face, thus when you inject, they bleed for longer and bruise. Consider working in clinic rooms with air conditioning or apply a cool compress to your patient’s lips before you start injecting.
Remember to screen your patients for those most susceptible to bruising – taking medication that thins the blood (aspirin, clopidogrel) or anticoagulants. Consider how you will manage these patients, and whether you want to treat them at all. You must consent them that they will be more likely to bruise, but you may also wish to treat them at a time that you can take longer with the procedure to ensure that you are stopping any bleeding with your hand and not looking to see if it has stopped bleeding too soon. A very simple tip from Dr Tim is to put your finger on any bleeder and do not look at it for at least 30 seconds, maybe a minute if it is on the bigger end of the scale because that is your chance to stop their blood leaking out, flooding the tissues, and causing a bruise.
Many patients think a bruise equates to an injury. This means that they will go home thinking “I have been injured by my clinician”, rather than “I have a blood vessel that had a needle passed through it and it leaked blood under the skin”. As medical professionals, we know how bruising happens, but most patients have never thought about it in any detail and associate it with being hurt. Thus, when you explain a bruise, they quite often feel a lot better when it occurs post treatment, and it does not mean that they have been assaulted!
You can find Dr Tim Pearce on Instagram if you have a question that you want him to answer on running an aesthetic practice.

Lip Filler Treatment & Complications
With all the conflicting advice out there about lip filler treatments – vertical or horizontal? needle or cannula? – it can be difficult to know how to inject to create the lips your patient desires.
If you are suffering from technique overwhelm, worrying about causing a vascular occlusion (VO), or panicking about injecting thin lips, then Dr Tim Pearce’s brand-new ultimate lip course is going to teach you the different techniques, anatomy, and skills you need to create medically beautiful lips.
Aesthetics Mastery Show
For more insight, watch the latest episode of the Aesthetics Mastery Show, where Dr Tim shares 6 expert tips on how to stay safe and avoid complications when injecting the lips.
Is your worst nightmare causing a VO?
If you want to be a great injector then you need to get over your fear of complications. Register here for the next webinar to help you overcome your complications anxiety >>
Subscribe to our YouTube channel for really useful regular tips and advice. ![]()
Dr Tim Pearce eLearning
Dr Tim Pearce MBChB BSc (Hons) MRCGP founded his eLearning concept in 2016 in order to provide readily accessible BOTOX® and dermal filler online courses for fellow Medical Aesthetics practitioners. His objective was to raise standards within the industry – a principle which remains just as relevant today.
Our exclusive video-led courses are designed to build confidence, knowledge and technique at every stage, working from foundation level to advanced treatments and management of complications.
Thousands of delegates have benefited from the courses and we’re highly rated on Trustpilot. For more information or to discuss which course is right for you, please get in touch with our friendly team.
Related Articles
 Bestseller
Bestseller
Why Everything we’re Doing for Skin, Hair, and Weight May Not Translate Clinically
April 21, 2026
 Bestseller
Bestseller
Why One Milliliter of Lip Filler Can Ruin Small Lips
April 16, 2026