- Mail us: support@drtimpearce.com
How to reduce risk and avoid vascular occlusion with dermal fillers
You may be interested
 Dr Tim Pearce
Dr Tim Pearce

How do you approach risk when treating a patient’s face? It is true that everywhere that you can inject has some inherent risk – the simplest way to reduce that risk down to zero is by not doing the procedure, but you also reduce the benefit to the patient down to zero. As medical professionals we must constantly justify the risk we take against the intended benefit for our patients, focusing on the health of our patients as the intended outcome of medical aesthetic treatments.
In this blog, Dr Tim Pearce will explore several ways that you can reduce risk, primarily the risk of vascular occlusion (VO), breaking it down into the two elements that we can control – the frequency of vascular occlusion and the severity of vascular occlusion.
Do you feel anxious about causing complications? Many clinicians feel so overwhelmed with the thought of causing a vascular occlusion that it stops them growing their aesthetics business. Dr Tim is currently hosting a webinar series to help you overcome your fear of complications so that you can uplevel your knowledge, and increase your CPD-certified learning to build a successful aesthetics business. Sign up here >>
Understanding the risk of vascular occlusion – frequency and severity
 The overall risk is of a vascular occlusion injury, in other words not just the risk of a vascular occlusion happening, but the resulting injury. We have factors that affect the frequency of vascular occlusion occurrence, factors that affect the severity (of the injury), and then there is your ability to diagnose and treat a vascular occlusion if it does occur. These are the three factors which guide all our safety in medical aesthetics.
The overall risk is of a vascular occlusion injury, in other words not just the risk of a vascular occlusion happening, but the resulting injury. We have factors that affect the frequency of vascular occlusion occurrence, factors that affect the severity (of the injury), and then there is your ability to diagnose and treat a vascular occlusion if it does occur. These are the three factors which guide all our safety in medical aesthetics.
The frequency of vascular occlusion is how likely it is to get dermal filler into a vessel whilst injecting and performing a particular procedure. The severity of vascular occlusion is determined by how big the problem becomes in terms of vascular compromise and injury by depositing filler into a vessel.
These two elements of risk are in direct competition – quite often we will do something that decreases the frequency risk, or likelihood of a VO, but a particular technique may increase the severity risk and injury if a VO were to occur; conversely, we may do the opposite. There is much debate on balancing this risk in medical aesthetics.
Can moving the needle reduce the risk of vascular occlusion?
Dr Tim reports that some practitioners have recently been recommending moving the needle as a way of reducing the risk of causing a VO. Inherently, in the logic of this option, you will increase the frequency of vascular occlusion occurrence, but this is claimed to be offset by the decrease in the potential severity due to movement – injecting small amount of products over a wide area will risk more VOs but each will be much smaller. The exact parameters surrounding this are not well defined and are highly debatable, warns Dr Tim, so he does not regard it as good advice.
What affects the frequency of vascular occlusion?
Dr Tim believes that there are four factors that affect the frequency of vascular occlusion occurrence in clinic.
- The proximity of your needle tip to a named vessel – think about named vessels near areas you commonly treat.
- The ease with which, using your technique, you could place the needle into the lumen of a vessel – think about the depth and orientation of your needle relative to the orientation of the vessels in the area.
- The amount of tissue that is exposed to the needle tip in a procedure – moving the needle would increase the frequency of risk.
- The regularity with which you perform a procedure – if it is a common procedure, your risk as an injector is higher than with a very rare procedures that might be more dangerous.
How to reduce the risk of causing a vascular occlusion when injecting filler
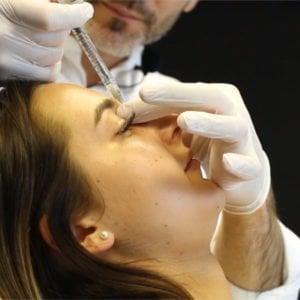 Breaking it down, we can think about the areas of the face that you inject most frequently when your needle is parallel or oriented in the same direction as a vessel, and when you are only millimetres away from a vessel.
Breaking it down, we can think about the areas of the face that you inject most frequently when your needle is parallel or oriented in the same direction as a vessel, and when you are only millimetres away from a vessel.
For most aesthetic clinicians, this equals the lips, the most common area in which to cause a vascular occlusion, particularly in the top lip. The (good) thing about lip VOs is that they are usually the easiest to diagnose, the chance of a lip VO going undiagnosed is much less than in other areas of the face because lips are normally pink, and it is easy to see if they go pale. Lips also have a high density of nerve receptors; thus, pain is likely to be an early diagnostic signal with patients readily seeking advice.
Honing your skills when it comes to understanding and visualising lip anatomy, your injection technique, and other steps like aspirating will help you to reduce the risk of causing a vascular occlusion in the lip.
Other areas of VO risk include treating the dorsum of the nose, particularly if you use a cannula because you are in parallel with the dorsal nasal arteries, the nasolabial fold, and when injecting the lower face near the mental and submental arteries.
What affects the severity of vascular occlusion
Dr Tim believes that there are three factors that affect the severity of a vascular occlusion if you were to get one in clinic.
- How much are you injecting into a given area?
- What is your proximity to major vessels, particularly where they are at their largest?
- What is your proximity to any major structures that we do not want to affect with a vascular occlusion – the eyes, brain etc?
The area where you a most likely to cause a severe injury with a vascular occlusion – with a combination of volume (of filler) and proximity to major vessels that supply the eye and the brain – is when treating the nasion (the area between the forehead and the nose). Practitioners will often add 0.5ml of filler or more into the area to straight the nose.
In summary, the most likely place to get a severe vascular occlusion is in the nose, and the most frequent place to get a vascular occlusion is in the lips, particularly the top lip.
Which vessels are at risk from blockage by large volumes of dermal filler?
The roots of the arteries, (where they enter the face), and where they are at their thickest, alongside how often you tend to inject around those points increase the likelihood of a severe vascular occlusion. There are five areas where vessels enter the face that Dr Tim highlights at particularly risky for severe VO with large volume filler deposits.
- The facial artery, where it enters the face at the mandible and as you get closer to the medial face, the nasolabial fold is an area of concern.
- The submental and mental arteries in the lower third of the face.
- The infraorbital artery.
- The supratrochlear artery.
- The superficial temple and deep temple arteries.
In Dr Tim’s personal experience, the sliding scale of the most frequent areas that he injects that could be of higher risk is the nasolabial fold, followed by the temple and forehead, then the lower third of the face where he injects the chin and the medial labial fold.
Learn how to avoid 5 parallel arteries when injecting facial filler and do not inject filler deeply in these 6 danger areas of the face.
Reduce your risk of causing a vascular occlusion with these three questions
The risk of causing a VO will vary depending on your practice, which instruments you use, your style of injection, and how frequently you perform different procedures. Dr Tim therefore has three questions that he recommends you ask yourself that will help you to become a safer injector over time.
- What are the filler treatments that you do most frequently? Focusing your attention on becoming safer with those procedures will likely give you a disproportionate reward in terms of reducing risk, so get really focused on the detail, learn about the different positions of the arteries in their areas, and specifically learn about the depths and locations, how you can locate them before you inject by palpating the area, using ultrasound, or learning the different variations of anatomy down to the millimetre.
- What can you do to reduce the probability of a vascular occlusion? This does not mean the size of a VO; it is anything that you can do that would decrease the total number of small amounts of filler that get into a vessel. For example, by knowing your anatomy, and knowing that the artery is never found at a particular depth according to studies that will tell you that you can inject there and decrease the frequency of VO. Similarly, another could be always aspirating, knowing that aspiration is not 100% sensitive but doing it routinely can increase the chance that you detect intravascular placement before you inject. Have a read of these blogs: does aspirating work? and how many seconds should you aspirate when injecting fillers?
- How do you reduce the severity of a vascular occlusion? This is largely about reducing the amount of filler that gets injected into the wrong place during treatment. Separating out the volumes as you inject, into small aliquots at a time allows you time to validate that there is no VO in between each injection. Similarly, this is where moving the needle could be seen to be of benefit, as you distribute the filler more widely, although you risk increasing the frequency of VO occurrence.
The different ways you can achieve this are numerous, but Dr Tim urges you to think about it and apply it to your day-to-day practice. Overall, as you start to answer these questions, you will start to feel that there is no perfect solution, everything has a potential upside and a downside, and we are constantly trying to balance those factors. If you are continually asking yourself these questions then you will be heading in the direction of increased safety; if you never ask these questions, you may start to drift in a completely wrong direction and increase the overall risk for your patients.
You can find Dr Tim Pearce on Instagram if you want to drop him a comment or question to discuss aspiration or other patient safety techniques for performing dermal fillers.
Is your worst nightmare causing a VO?
If you want to be a great injector then you need to get over your fear of complications. Register here for the next webinar to help you overcome your complications anxiety >>
Subscribe to our YouTube channel for really useful regular tips and advice. ![]()
Aesthetics Mastery Show
FILLER RISK: How to Avoid Vascular Occlusion
In this episode, Dr Tim explores every injector’s worst nightmare – occluding a vessel with dermal filler and possibly causing their patient harm. He then breaks down ways you can reduce the risk of vascular occlusion, and increase the likelihood of a good night’s sleep!. Watch the full Aesthetics Mastery Show here.
Robin Power commented on the video saying:
“ultrasound pre-treatment all day long. More information specific to the patient = safety. :)”
Robin Power
You can find out more about ultrasound in our features:
- Does ultrasound provide the evidence to support aspirating with fillers?
- Should I buy an ultrasound scanner for my aesthetic clinic?
Read more and join in the debate on our YouTube channel.
Filler Complications eLearning Courses
If you want to increase your confidence by learning how to handle complications, Dr Tim Pearce offers two comprehensive courses that are highly rated by our delegates:
Both give CPD and certificates on completion.
In addition, browse our FREE downloadable resources on complications.
Dr Tim Pearce eLearning
Dr Tim Pearce MBChB BSc (Hons) MRCGP founded his eLearning concept in 2016 in order to provide readily accessible BOTOX® and dermal filler online courses for fellow Medical Aesthetics practitioners. His objective was to raise standards within the industry – a principle which remains just as relevant today.
Our exclusive video-led courses are designed to build confidence, knowledge and technique at every stage, working from foundation level to advanced treatments and management of complications.
Thousands of delegates have benefited from the courses and we’re highly rated on Trustpilot. For more information or to discuss which course is right for you, please get in touch with our friendly team.
Related Articles
 Bestseller
Bestseller
Hack Your Age, Hack Your Health
May 26, 2026
Hack Your Age, Hack Your Health
 Bestseller
Bestseller
PRP Series | Part 2: Supercharging the Signal
May 19, 2026









Comment (1)
Jimmy G
Jul 10, 2022Ι’m not that much of a online reader to be honest but your sites really nice, keep it up!
I’ll go aheɑd and bookmark your website to come back in the future.
Cheers
Comments are closed.