- Mail us: support@drtimpearce.com
Dangers Of Using Non-Reversible Dermal Filler Products
You may be interested
 Dr Tim Pearce
Dr Tim Pearce
Dr Tim Pearce recently reviewed a case study of a patient who experienced a vascular occlusion with necrosis from an injection of calcium hydroxylapatite (CaHA) dermal filler (Radiesse®).
The patient, Julie Bass Kaplan, herself a nurse, explained to Tim in a recent Instagram Live interview that during training on the product a decade ago, a fellow practitioner injected her nasolabial area resulting in product entering her infraorbital artery, occluding the blood supply to her cheek, and causing significant injury and scarring.
Necrosis from Radiesse, what can we learn?
In this blog, Dr Tim will look at the points of learning that we can all take from Julie’s experience, including the increased risks posed by this type of product and the stages of necrosis we should be looking out for as aesthetic practitioners.
Dr Tim will be discussing more medical aesthetic training tips as part of his upcoming webinar series, so if you’re looking to increase your CPD-certified learning and want to learn more skills to make you a better practitioner, then step one is to register for the free webinars by Dr Tim.








What are the significant risks from Radiesse?
When reviewing a complication case study, it is possible to extrapolate many different components which may have contributed towards the risk of the complication occurring. Additional insight into Julie’s case of necrosis was discussed in an episode of the Aesthetic Mastery Show.
Non-reversible product
In this case, it could be argued that the most significant risk was the use of a non-reversible product – calcium hydroxylapatite. There are times when a non-reversible product is appropriate for use, such as in a patient with a known allergy to hyaluronic acid (HA), but it is a significant step up in the risk profile to use CaHA. Aesthetic practitioners should ideally try to use reversible products as much as possible in clinical practice. Non-reversible products became popular due to their longer-lasting capabilities (12-18 months), however we now have reversible HA-based products which last equally as long, so the justification for using products which cannot be reversed is limited. Those interested in the use of Radiesse may wish to read this expert consensus paper published in 2020 on Managing intravascular complications following treatment with calcium hydroxylapatite.
Ease of injection
CaHA is quite thick in nature which means that aspiration is practically impossible. You simply cannot pull product back, especially with a primed needle. Crucially in this case study from a decade ago, aspirating before every dermal filler treatment was not as widely used or taught at it is today. Another issue with a thick product is the requirement for considerable extrusion force. Dr Tim notes that from his experience using CaHA, it reduced his feeling of control when delivering expected quantities into a given area, and he could not deliver it smoothly.
Needle length
This product is often supplied or used with a longer needle; however, the longer the needle the more chance of multiplying the inaccuracy of the delivery as you cannot adequately judge the depth of your injection. Short needles are regarded as safer by experienced clinicians.
Product quantity
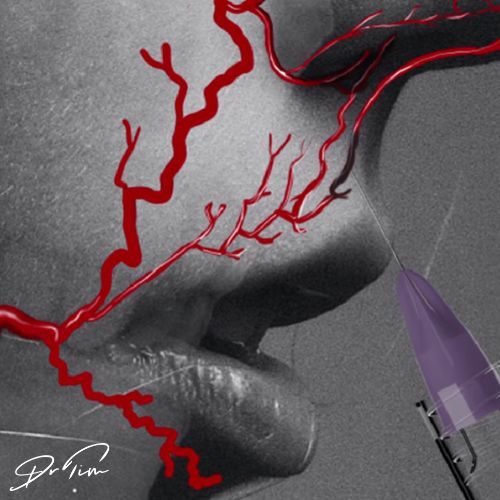
The amount of product injected at one entry point can have a notable impact of the severity of a complication. Although the likelihood of causing a vascular occlusion may be reduced by using fewer entry points, the larger the volume of product injected at a single point, the greater the severity of any resulting occlusion. In Julie’s case, 0.75ml of CaHA was injected into a location that was near crucial facial anatomy surrounding the infraorbital foramen.
Limited edition anatomy posters are available to buy for your aesthetic business as a helpful reminder of core vasculature.
Adding lidocaine and adrenaline
There are advantages to adding lidocaine and adrenaline to CaHA, for example, it can dilute the product somewhat and decrease the extrusion force, allowing for smoother injection. Lidocaine will also make the procedure more comfortable for the patient and adrenaline causes vasoconstriction which aids the local infiltration and maintenance of the anaesthetic effect.
Sadly, this practice also comes with disadvantages. Adrenaline can confuse diagnosis of a problem, as was the case with Julie. The resulting pallor on her skin post procedure was attributed to the adrenaline, with an expectation that it would quickly resolve. Similarly, lidocaine can also mask a problem as the patient feels no pain. Julie experienced no pain for six hours post treatment due to this numbing effect. Without anaesthesia, one would expect a patient to present with pain within two hours of a positive vascular occlusion.
In all fairness, the same problem could occur with a reversible product as many HA fillers now come with lidocaine within the pre-filled syringe, or where a so-called ‘dental block’ lidocaine infiltration is used. Aesthetic practitioners should be mindful that the patient may not always feel an impending complication due to anaesthesia, so you need to spot it first!
Stages of necrosis
-

Blanching – skin is pale and there is no capillary blood flow.
- Livedo reticularis or Mottling – skin has a mottled pattern with pale areas where no fresh blood is entering and a surrounding area of livedo or deoxygenated blood which is building up in the tissue to create a net-like appearance. This is short lived after the initial occlusion.
- Pustule formation – 24-36 hours later, pustules appear on the skin which are often confused with a herpes infection. Herpes rarely occurs on normal skin so practitioners should rule out a diagnosis of vascular occlusion before jumping to considering herpes simplex.
- Coagulation – skin starts to denature, appearing dry and non-reflective. Areas of black start to appear as the skin begins to solidify.
- Skin breakdown – tissue begins to liquify and slough off as enzymes are released which break down the collagen and elastin. This is the end of the necrotic stages.
It is important to note that not all stages of necrosis will manifest in the same way as you might see in textbook illustrations, teaching manuals, or on training days – using skills such as checking for capillary refill are vital if you suspect a vascular occlusion.
Dr Tim is grateful to Julie Bass Kaplan for detailing her experiences, you can follow Julie on Instagram for more insightful hints and tips.
NON-REVERSIBLE FILLER DANGER:
Dr Tim examines necrosis case post Radiesse
Still anxious about delivering cosmetic injectables safely?
If you want to learn more about mastering medical aesthetic treatments and complications, or conquering the anxiety of where to place your needle, then register for the next Dr Tim webinar.
Subscribe to our YouTube channel for really useful regular tips and advice. ![]()
Dr Tim Pearce eLearning
Dr Tim Pearce MBChB BSc (Hons) MRCGP founded his eLearning concept in 2016 in order to provide readily accessible BOTOX® and dermal filler online courses for fellow Medical Aesthetics practitioners. His objective was to raise standards within the industry – a principle which remains just as relevant today.
Our exclusive video-led courses are designed to build confidence, knowledge and technique at every stage, working from foundation level to advanced treatments and management of complications.
Thousands of delegates have benefited from the courses and we’re highly rated on Trustpilot. For more information or to discuss which course is right for you, please get in touch with our friendly team.
Related Articles
 Bestseller
Bestseller
Vermilion border vs wet-dry border: solving the labial artery confusion with 3D anatomy
April 9, 2026